Pediatric & Adolescent Concussions: A Parent’s Guide to Safe Recovery in Winnipeg
It happens in a split second: a collision on the ice at the hockey rink, a fall at the playground, or a tangled set of legs during a soccer match at the local soccer centre. As a parent, that moment of impact brings an immediate rush of worry. You aren’t just looking for a quick fix; you’re looking for the best way to protect your child’s developing brain and ensure they can safely return to the classroom and the field. Understanding concussions in children and adolescents is the first step in replacing that worry with a clear, evidence-based plan for recovery.
Source: Shutterstock
Why Concussion Care is Different for Children and Teens
In Winnipeg, our kids are active year-round—from summer league soccer to the intense pace of winter hockey and community center basketball. While physical activity is vital for development, it does come with the risk of concussions, which are among the most common injuries seen in Manitoba youth sports.
The Developing Brain and Recovery Timelines
At Better Beyond Rehabilitation, we understand that a "wait and see" approach can be frustrating for families. Parents often tell us they feel stuck between wanting their child to rest and worrying about them falling behind in school. Research published in journals like Pediatrics emphasizes that children’s brains are more vulnerable to injury and often require longer recovery periods than adults because their neurological systems are still developing. This is why a "one-size-fits-all" adult protocol does not work for a ten-year-old.
Common Myths: Why Your Child Doesn't Need to "Black Out"
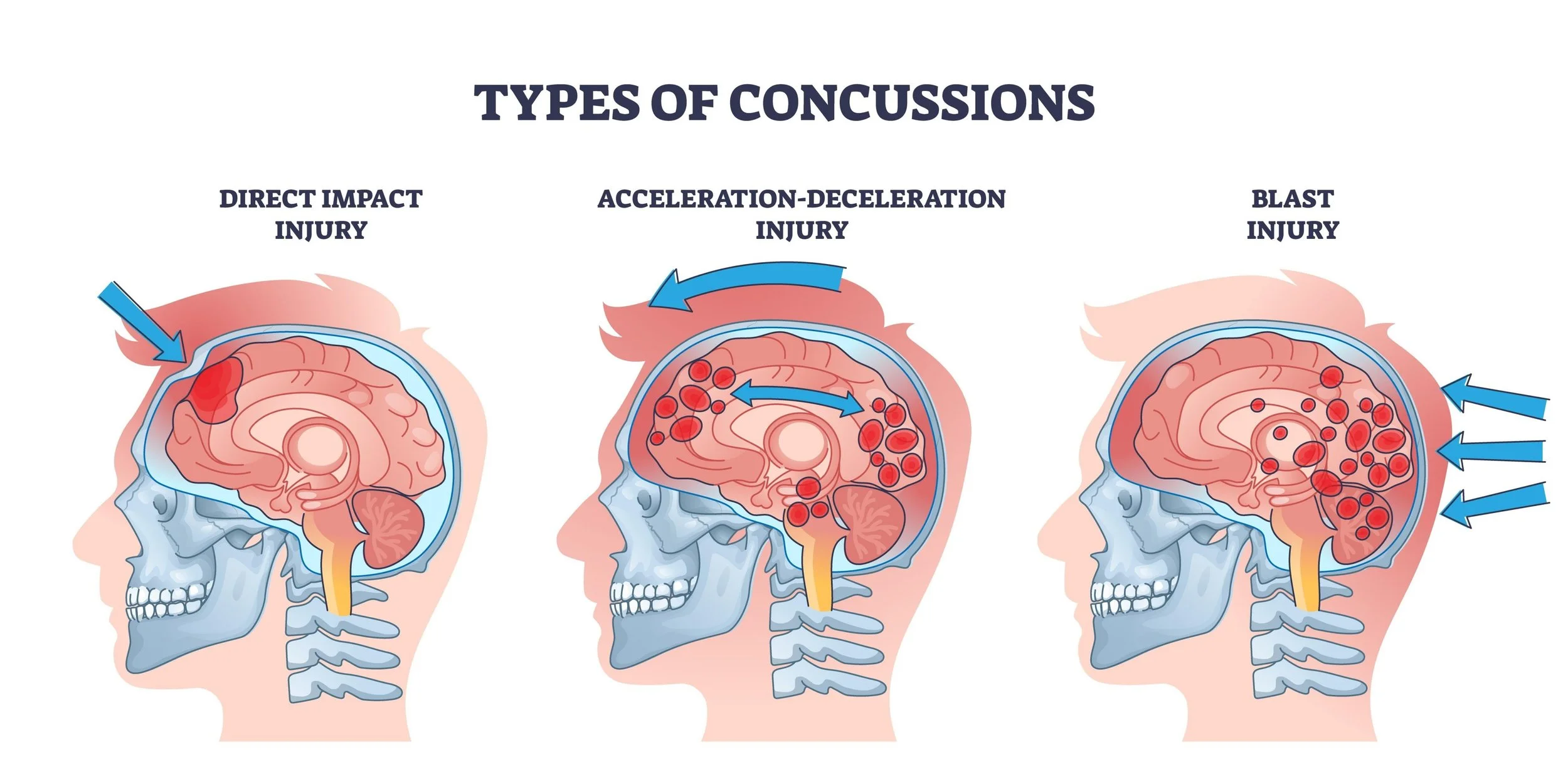
It is a common myth that a child must "black out" to have a concussion. In fact, the vast majority of pediatric concussions occur without any loss of consciousness. A concussion is a mild traumatic brain injury (mTBI) caused by a bump, blow, or jolt to the head or body that causes the brain to move rapidly back and forth inside the skull. This movement can create chemical changes in the brain and sometimes stretch or damage brain cells, even if the impact seemed minor.
Recognizing the Signs: What Every Parent Should Watch For
Concussion symptoms can vary significantly between children and may not appear immediately after the injury. Being able to identify these signs early helps in managing the recovery process effectively.
Physical Symptoms: Beyond Just Headaches
While a headache is the most reported symptom, keep a close watch for:
Dizziness or balance problems
Nausea or sensitivity to light and noise
Feeling unusually fatigued or "drained"
Blurred or double vision
Cognitive and Emotional Changes: The "Fog" and Irritability
The "invisible" symptoms are often the most distressing for teens. You might notice:
Difficulty concentrating or remembering new information
Feeling "foggy" or slowed down mentally
Increased irritability or unusual mood swings
Changes in sleep patterns (sleeping significantly more or less than usual)
Subtle Clues in Younger Children
Younger children may not have the vocabulary to describe "brain fog." In these cases, look for changes in play habits, excessive crying, or a loss of interest in their favorite toys or activities.
The Modern Approach to Recovery: Beyond the "Dark Room"
Outdated advice often recommended keeping a child in a dark room with no screens or activity for weeks. We now know that strict, prolonged rest can actually delay recovery and lead to increased anxiety or depression in adolescents.
The 24–48 Hour Rest Phase
Current clinical guidelines suggest a brief period of physical and cognitive rest for the first 24 to 48 hours. This means a break from sports, intense schoolwork, and excessive screen time to allow the initial "energy crisis" in the brain to stabilize.
Moving From Total Rest to Active Rehabilitation
Once that initial window passes, the focus shifts to active recovery. Research shows that light, sub-symptom physical activity—like a gentle walk—can actually help the brain heal faster.
Targeted Therapies: Eyes, Neck, and Balance
At our Seasons of Tuxedo clinic, we focus on identifying the specific "driver" of the symptoms:
Vestibular & Oculomotor Therapy: We assess how the eyes and inner ear communicate. If your child feels dizzy when reading, specific eye-tracking exercises can help manage these symptoms.
Cervical Spine Assessment: Many concussion symptoms overlap with "whiplash-style" neck strain. Addressing neck tension in our clinical space can often alleviate persistent headaches.
Navigating the Return to School and Sport
The goal is to get your child back to their normal life, but the order in which we do this matters.
"Return-to-Learn": Prioritizing the Classroom
A "Return-to-Learn" plan should always be successfully managed before a child returns to full-contact sports. This might include temporary school accommodations like reduced workloads, extra time for assignments, or scheduled rest breaks during the school day.
The Step-Wise Protocol for Returning to Play
We follow a structured, step-by-step protocol. Your child will move from light aerobic exercise to sport-specific drills, and eventually to non-contact practice, only progressing to the next stage if they remain symptom-free. This reduces the risk of repeat concussions and long-term complications.
When to Seek Professional Support at Better Beyond Rehab
If your child has sustained a hit and is struggling to return to their normal routine, a professional assessment is a vital next step. We provide the objective testing needed to determine when it is safe to increase their activity levels.
Red Flags: When to Seek Emergency Medical Care
Please seek immediate emergency medical attention at the nearest hospital if your child experiences:
A headache that gets significantly worse and does not go away
Repeated vomiting or nausea
Seizures or tremors
One pupil appearing larger than the other
Increasing confusion, agitation, or slurred speech
Key Takeaways for Winnipeg Families
Act Early: Early assessment helps identify the specific rehabilitation needs of your child.
Classroom First: Ensure your child can handle a full day of school before they return to the ice or field.
It Takes a Village: We work alongside parents, coaches, and teachers to ensure the recovery plan is consistent.
Stay Positive: Evidence suggests that with the right management, most children experience a full recovery and return to the activities they love.
Navigating a child’s recovery can feel overwhelming, but you don't have to do it alone. A physiotherapy assessment can help identify the contributing factors to your child's symptoms and provide a clear, step-by-step plan for the weeks ahead. If you have questions about your child's recovery, visit our booking page to schedule an assessment at our Seasons of Tuxedo clinic.
This information is for educational purposes and is not intended to replace professional medical advice. If your child is experiencing symptoms of a concussion, consult with a qualified healthcare provider for an assessment tailored to their specific situation.
Sources:
McCrory P, et al. Consensus statement on concussion in sport. British Journal of Sports Medicine.
Parachute Canada: Canadian Guideline on Concussion in Sport.